Duodenal Atresia
What is Duodenal Atresia?
Duodenal atresia can be defined as a congenital problem, in which a part of the duodenum lumen is absent or completely closed. Also known as duodenojejunal atresia, this condition leads to the accumulation of amniotic fluid during the prenatal period. It is also responsible for complications such as intestinal obstruction, which can affect newborns. Upon performing imaging studies, such as X-rays, the stomach will appear distended and so will the duodenum. As you will have the opportunity to read below, the separation of the stomach from the duodenum is physiologically made by the pyloric valve, hence the double-bubble sign on the X-ray.
Duodenal atresia is believed to appear in 1 in every 5000-10000 live births, with 20-40% of all the born babies suffering from Down’s syndrome. No gender prevalence has been identified so far. Studies have shown that almost 8% of all the infants diagnosed with Down’s syndrome also suffer from duodenal atresia. Apart from Down’s syndrome, duodenal atresia is often associated with other birth defects (VACTERL, annular pancreas, jejuno-ileal atresia, ileal atresia or anal atresia). Other associated birth defects are present at the level of the heart or within the genitourinary tract. This condition is known to be one of the most common causes that leads to the appearance of fetal bowel obstruction. It can be however corrected in the neonatal period.
There are children who are born prematurely because of this condition. Upon being born, many of the children who suffer from duodenal atresia appear to be completely healthy. However, the symptoms because obvious when they are fed, with green vomiting raising the suspicion for the diagnosis. Duodenal atresia is often confirmed through imaging studies (X-rays in particular).
Symptoms
The symptoms of duodenal atresia are present during and after the pregnancy. It is important to understand that duodenal atresia can lead to increased quantities of amniotic fluid in the uterus, a condition which is known as polyhydramnios. This occurs as the fetus is unable to swallow the amniotic fluid, with a poor absorption at the level of the digestive tract.
Once the baby has been born, he/she will present abdominal distension and bilious vomiting as primary symptoms. The distension is mainly presented at the level of the upper abdomen, while the vomiting contains high quantities of bile acid. Due to the duodenum not having developed properly, the stomach contents cannot pass through the pyloric valve, leading to vomiting. The vomiting often occurs in large amounts and is not necessarily correlated to the feeding times (the infant can vomit hours after a meal). Apart from these symptoms, both the urination and the bowel movements can be absent (in the situation of urination, after the first few voidings; as for the bowel movements, the absence is noticed after the first few meconium stools).
If the condition is left untreated, serious dehydration can occur, with important electrolyte imbalance. Without treatment, duodenal atresia can lead to life-threatening symptoms.
Causes
Despite the extensive research made in the field, the exact cause that leads to the appearance of duodenal atresia has yet to be identified. At the moment, it is believed that the main cause behind this congenital problem is a defect in the development of the embryo. Basically, the duodenum does not change its structure, leading to the respective problems.
Other scientists consider that the main cause of duodenal atresia is the damage that occurs at the level of the duodenum in the fetal period, due to the loss of blood supply. This can cause the structure of the duodenum to become modified, as this part of the intestinal tract is narrower and obstructed.
Pictures of Duodenal Atresia
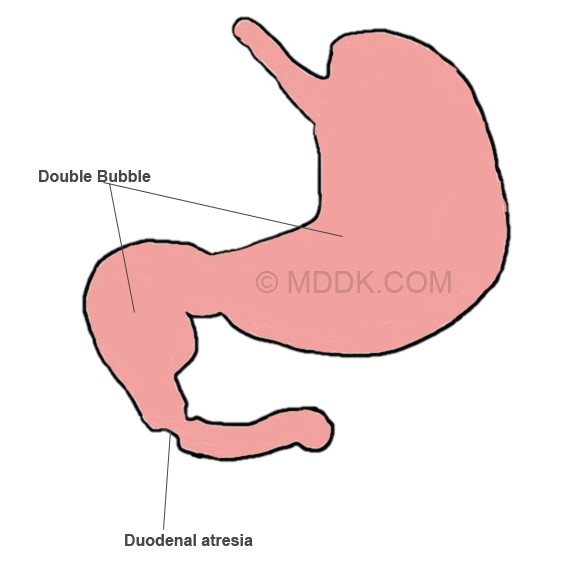
Picture of Duodenal atresia showing the Double bubble sign
Diagnosis
These are the most common methods used for the diagnosis of duodenal atresia:
- Imaging studies
- X-ray – double bubble sign – the air is trapped in the stomach and proximal part of the duodenum, with the pyloric valve separating them (due to the atresia, the distal part of the duodenum does not contain trapped air)
- Physical examination
- Patient history – information on the pregnancy
- Blood testing – check for electrolyte imbalance.
During the pregnancy, duodenal atresia can be diagnosed with the help of the fetal ultrasound. Excessive amounts of amniotic fluid can be identified at the level of the womb; the ultrasound can also reveal the distension in the upper part of the abdomen. Unfortunately, this condition is cannot be diagnosed until the second half of the pregnancy. Moreover, its signs cannot be seen until the third semester of pregnancy. The increased quantities of amniotic fluid suggest a risk of pre-term labor, with the mother-to-be being closely monitored for such problems.
Differential diagnosis can be made with the following conditions: duodenal stenosis, duodenal web, intestinal malrotation, midgut volvulus (plain film appearance). In regard to the ultrasound appearance, the differential diagnosis can be made with: fetal choledochal cyst, fetal omental cyst and fetal enteric duplication cyst.
Treatment
These are the most common treatment approaches used for duodenal atresia:
- Fluid removal from the stomach with the help of a nasogastric tube
- Administration of intravenous fluids (to prevent dehydration and correct electrolyte abnormalities)
- Surgical intervention
- Open or laparoscopic approach
- Surgical repair of the intestinal closure
- Not an emergency intervention
- Reduced morbidity and mortality rate with the initial repair
- A second intervention might be necessary.
Aside from the surgical intervention, there aren’t other alternatives for correcting the defect at the level of the duodenum.
The risks of the surgical intervention include:
- Small risk of bleeding
- Damage to the nearby structures of the abdomen (very rare)
- Leakage of bowel contents into the abdomen (risk of infection – antibiotics are administered as a prophylactic measure; might require a second surgical intervention)
- Anesthesia-related complications.
After the surgery, it may require some time for the bowels to start functioning properly. During the recovery period, it is highly likely that the child will be fed with the help of parenteral nutrition. Immediately after the operation, the vital signs (breathing, heart rate and oxygen levels) are closely monitored. A ventilator might be connected, so as to assist the baby with the breathing process. Pain medication is administered through the intravenous infusion.
In the situation that this condition is identified during the pregnancy, genetic counseling is recommended – a specialist can discuss the most essential aspects related to genetic abnormalities and how they can influence the health of the future baby. Moreover, if there are increased quantities of amniotic fluid, a procedure known as amnioreduction can be performed. This procedure will reduce the risk of pre-term labor and it will also improve the breathing in the mother.
Prognosis and Complications
In the majority of the patients, the prognosis is positive, with no complications present. However, the risk of complications is higher when there are other congenital anomalies present. It is also possible that complications due to the duodenal atresia occur later in life, with a 6% mortality rate for these patients being identified. The late complications that can occur after the surgical intervention include: gastroesophageal reflux, problems regarding the bowel movements and inflammation of the proximal duodenum (condition known as megaduodenum). The complications of the surgery can also lead to significant feeding and absorption dysfunctions. After the surgery, the baby might present increased requirements for vitamins, such as those from the B12 complex.
Once a child has gone through surgical intervention for duodenal atresia, regular check-ups are essential with the passing of time. The check-ups are required, so as to ensure that the child grows and develops within standard. The loss of intestinal tissue can also lead to nutritional deficiencies, so the child has to be monitored for that as well. The progress of the child is influenced not only by the remaining length of the intestine but also by the association of other defects or abnormalities. A multidisciplinary team can assess the progress of the child as he/she grows older.