Urticaria Pigmentosa
Urticaria pigmentosa is a skin disorder in which the skin presents patches of dark color and the patient experiences intense itchiness. Rubbing or scratching the lesions can lead to the appearance of hives. This skin condition is also known as the generalized eruption of cutaneous mastocytosis and it most often affects children. Mastocytosis is a rare skin condition in which the number of mastocytes is excessive.
The mastocytes are the cells responsible for the elimination of histamines in case there is an allergen breaching into the body. Being diagnosed with any form of mastocytosis means that patient is more susceptible to serious allergic reactions, ranging from urticaria pigmentosa to severe anaphylactic shock.
Urticaria Pigmentosa Symptoms
These are the most common symptoms of urticaria pigmentosa, caused by the excessive amounts of mast cells present in the skin:
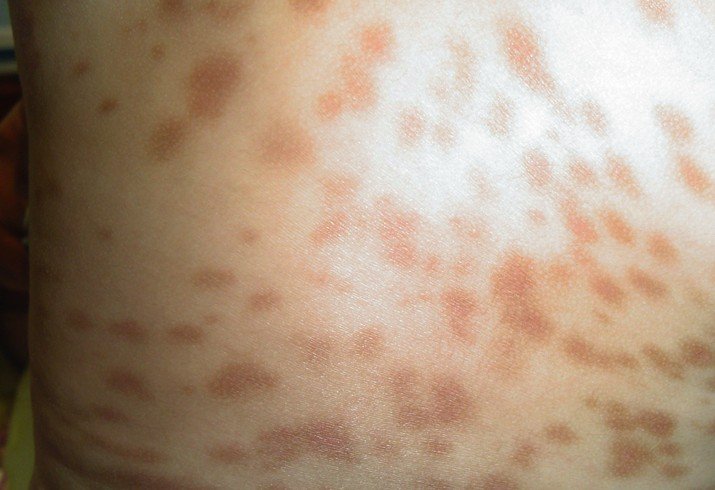
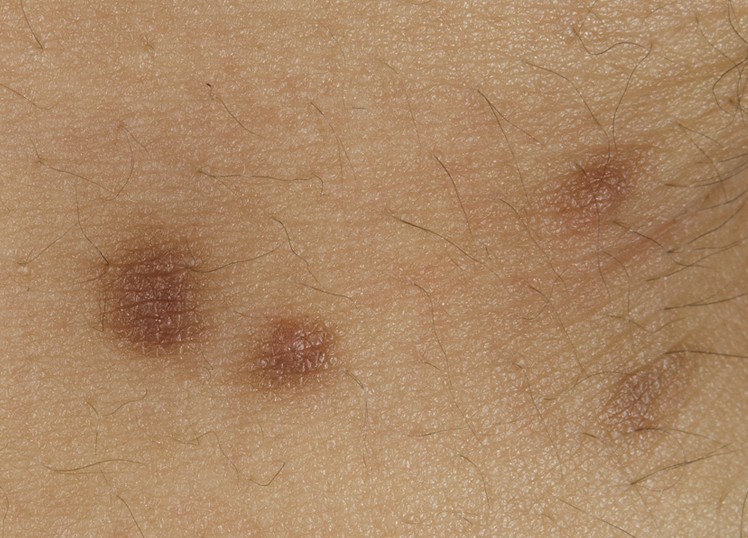
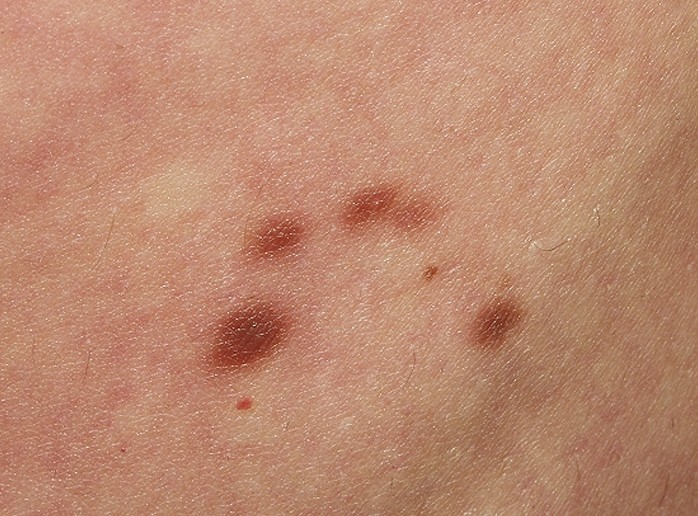
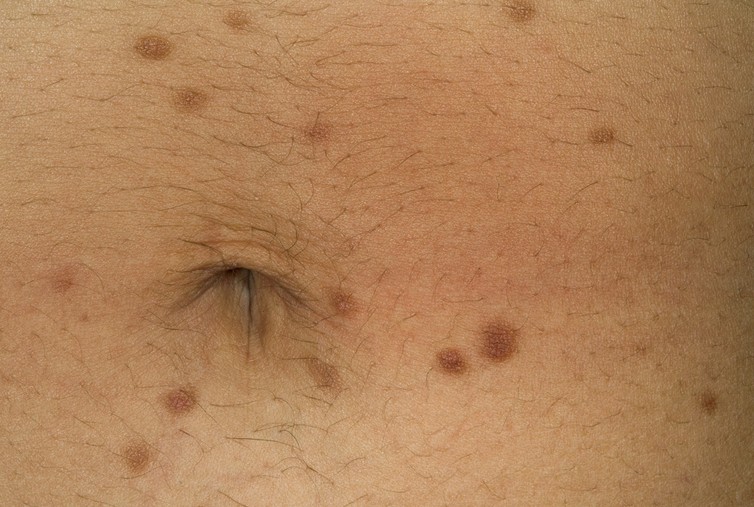
- Red or brown spots or patches present on the skin
- Patches are initially confused with moles or insect bites
- Lesions persist and increase in number over the course of years
- The areas that are most affected – chest, back and forehead
- Darier’s sign – stroking the skin in a particular area will cause inflammation, redness and itchiness (histamine response)
- Scratching can aggravate the condition and can also lead to the formation of blisters filled with liquids in children
- Flushed face in certain cases
Symptoms can vary considerably from one person to the other:
- Mild – redness, irritation
- Moderate – accelerated intestinal transit, cardiac pulse changes, nausea, vomiting, headaches and fainting
- Severe – anaphylactic shock, with difficult breathing and vascular collapse. This requires emergency medical treatment.
Possible Causes of Urticaria Pigmentosa
Urticaria pigmentosa appears in people who have too many mast cells in their skin. The main cause is determined by the mutation of an amino acid, this in turn leading to the division of more and more mast cells. Several mutations have been incriminated into the appearance of urticaria pigmentosa and it seems that each mutation leads to a different time of appearance for the skin condition. Familial cases of urticaria pigmentosa have also been identified in the medical literature. Patients who have received radiotherapy as a treatment for breast cancer have also developed certain forms of urticaria pigmentosa. Two other conditions have been linked: HIV infections and disorders of the autism spectrum.
It is believed that there are many triggering factors that can also cause the condition to manifest itself. These are:
- Stress
- Emotion
- Anxiety
- Physical exercise
- Excessive heat
- Skin friction
- Bacterial infections
- Venom from different animals
- Eye drops containing allergenic substances
- Anti-inflammatory drugs – aspirin is one of the most controversial triggering factors, as a certain amount of the drug will prevent the cells from dividing while a bigger amount will cause a histamine response.
- Alcohol
- Treatments with morphine.
Treatment
The treatment for urticaria pigmentosa is aimed to provide relief from the symptoms experienced, both at the level of the skin and also at a systemic level. The recommended is that all substances that might trigger an allergic response and thus the release of histamine should be avoided. As for the conservative treatments, they are as it follows:
- Antihistamines – these are recommended in order to reduce the itchiness, alleviate the flushing and also improve the symptoms experienced in the gastrointestinal tract.
- Oral disodium cromoglycate – this is recommended for patients who experience both cutaneous and systemic symptoms. This medication can be used in order to ameliorate the itchiness and the flushing at the level of the skin but also to improve the systemic symptoms, such as the accelerated intestinal transit, the abdominal cramps and other similar problems.
- Aspirin – this is recommended in a certain dose in order to maintain the mast cell degranulation. It is especially indicated in patients who have shown resistance to antihistamines but one must be careful as a high dose of aspirin could aggravate the symptoms of urticaria pigmentosa and even induce vascular collapse.
- Topical corticosteroids are recommended for cutaneous symptoms restricted to smaller areas.
- Intralesional injections with corticosteroids are recommended in more serious cases but the treatment cannot be performed for prolonged periods of time, as there is an increased risk of skin atrophy.
- Systemic corticosteroids are recommended only in severe cases, where there are other medical problems present, including malnutrition, liver disease or grave skin disorders.
- Oral psoralen in combination with UV-A therapy has shown promising results, improving the appearance of the skin affected by the lesions. However, prolonged treatments of this kind increase the risk for skin cancer.
- Immune modulators
- Patients who know that they present an increased risk for anaphylactic shock should wear medical alert braces and they should always have an epinephrine self-injector with them.
Urticaria Pigmentosa Pictures
Collection of photos and pictures of Urticaria Pigmentosa…