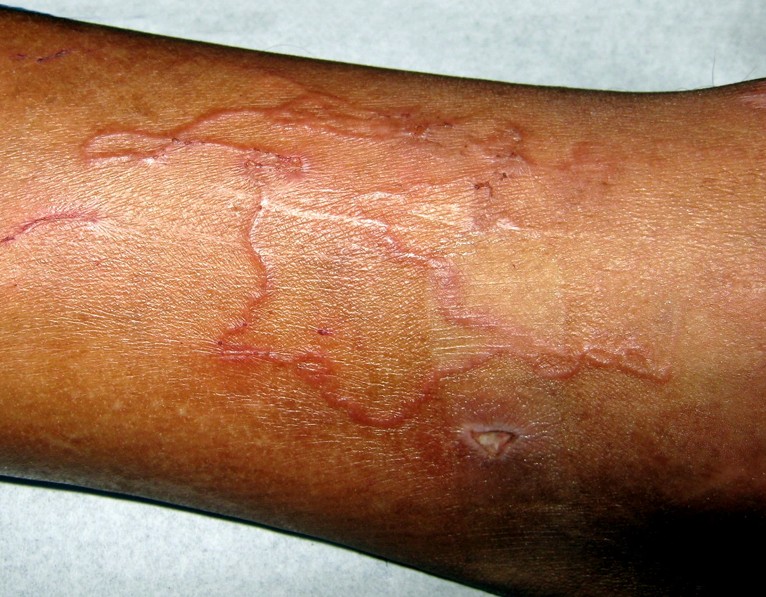
Cutaneous Larva Migrans
Cutaneous larva migrans is a type of dermatitis that occurs in people who have traveled to tropical and subtropical geographical areas. However, because more and more people travel in different areas on the globe, the infection is no longer confined to these areas. The skin presents an eruption that is accompanied by redness and intense pruritus. What happens is that the larvae of different parasites penetrate the skin and migrate from one areas of the body to the other. The eggs of the parasite are passed from the feces of animals into the soil and then the larvae start searching for a new host.
The infection with these larvae often happens when there is a breakdown in the skin, such as a cut or abrasion. However, the larvae can penetrate through the hair follicle and even through intact skin. Migration begins several days after the cutaneous penetration has occurred. This condition is more often encountered in animals and humans are only accidental hosts. This is a benign condition and it is strictly limited to the area of infection. The most disturbing symptom of cutaneous larva migrans is the intense itchiness. There is no gender prevalence and, when it comes to the age, it seems that children are more often affected than adults.
Symptoms of Cutaneous Larva Migrans
These are the most common symptoms of cutaneous larva migrans:
- Tingling sensation
- This appears half an hour after the skin penetration
- It may also be described as a prickling sensation
- There are also cases where the onset is late
- Intense itchiness
- The penetrated area is red
- Lesions might form a straight line or even a serpiginous tunnel; when a tunnel is formed, it is a little bit elevated
- Continuous advancement of the lesions (line or tunnel)
- Lesions in the form of papules or vesicles
- When vesicles form on the skin, these are filled with serous liquid
- Systemic involvement:
- Peripheral eosinophilia (Loeffler syndrome)
- Migratory pulmonary infiltrates
- Increased immunoglobulin E (IgE) levels
- Areas that are most affected include:
- Lower extremities
- Dorsum of the feet
- Interdigital space of the toes
- Ano-genital region
- Buttocks
- Hands
- Knees
- Secondary infections can appear due to the excessive scratching
What are the Causes of Cutaneous Larva Migrans?
These are the most common parasites that lead to the appearance of cutaneous larva migrans:
Ancylostoma braziliense
- Type of hookworm, commonly found in domestic animals
- Present in the following geographical areas:
- United States (central and southern)
- Central America
- South America
- Caribbean
Ancylostoma caninum
- Type of hookworm, commonly found in dogs
- Present in Australia
Uncinaria stenocephala
- Type of hookworm, commonly found in dogs
- Present in Europe
Bunostomum phlebotomum
- Type of hookworm, commonly found in cattle
Other parasites (rare cases):
- Ancylostoma ceylonicum – type of hookworm, commonly found in cats and dogs
- Ancylostoma tubaeforme – type of hookworm, commonly found in cats
- Ancylostoma duodenale – type of hookworm, commonly found in humans, cats and dogs
- Necator americanus – type of hookworm, commonly found in humans
- Strongyloides papillosus – parasite commonly found in cattle, sheep and goats
- Strongyloides westeri – parasite commonly found in horses
- Pelodera strongyloides – parasite commonly found in dogs, cows, horses, sheep, guinea pigs and humans.
How is Cutaneous Larva Migrans Diagnosed?
These are the most common methods for the diagnosis of cutaneous larva migrans:
- Clinical examination
- Reveals characteristic appearance of the lesions
- Travel history
- Patients often declare having traveled in tropical or subtropical areas, performing different activities such as sunbathing or walking barefoot on the sand (exposure to the parasite eggs)
- Complete blood count
- Peripheral eosinophilia
- Increased immunoglobulin E (IgE) levels
- Skin biopsy
- May identify the actual larva
- Other modifications include:
- Creation of basal layer tracts
- Creation of under-the-skin burrows
- Spongiosis – the epidermal layer of the skin presents vesicles
- Keratin cells are necrotized
- The epidermis and the upper layer of the dermis are inflamed and infiltrated with increased levels of eosinophils
- Optical coherence tomography
- The larva can be identified in the epidermis
- Recommended for removal purposes
Differential diagnosis can be made with the following medical conditions:
- Impetigo
- Tinea pedis
- Contact dermatitis
- Dermatophytoses
- Erythema chronicum migrans (commonly associated with Lyme disease)
- Photoallergic dermatitis
- Scabies
Treatment for Cutaneous Larva Migrans
The treatment is recommended in order to relieve the symptoms (itchiness) and also to treat the secondary infections. Prevention is recommended and people traveling to tropical and subtropical areas are indicated to avoid walking barefoot on different types of soil (because of the potential contamination with hookworm eggs).
The following courses of treatment are recommended:
Antiparasitic agents
- Thiabendazole
- Topical application – early and localized lesions
- Oral administration – this is recommended in case of extensive lesions or if the topical treatment does not provide the desired results
- Albendazole
- Benzimidazole drug commonly recommended as treatment for infestations with parasitic worms
- Better tolerated than Thiabendazole
- Mebendazole
- Generally recommended for parasitic infestations, including the one with hookworms
- Oral administration
- Low toxicity drugs, easily absorbed into the bloodstream
- Ivermectin
- Broad-spectrum anti-parasitic drug
- Commonly recommended for parasitic infestations, including hookworms and other intestinal worms
- Kills the larvae but not the adult worms
- Potential side-effects include neurotoxicity (the central nervous system is depressed and ataxia can occur, among other serious symptoms)
- Oral or injectable administration
- Contraindicated in children and in women who are breastfeedings
Antibiotic therapy
- Recommended in case of secondary infections caused by excessive scratching
Cryotherapy
- Liquid nitrogen is used on the larval burrow
- Other choices for freezing include: Ethylene chloride spray and Solid carbon dioxide
- This procedure presents increased risk of blistering or ulceration
Anti-itchiness cream
- Relieves the intense pruritus
- Topical corticosteroids – hydrocortisone cream
- Calamine lotion – this has a soothing effect for the skin, relieving the itchiness and also reducing the inflammation
Anti-histamines
- Oral or topical administration
- Recommended to relieve the intense itchiness and other upsetting symptoms
Cutaneous Larva Migrans Pictures
Collection of photos, images and pictures of Cutaneous Larva Migrans…