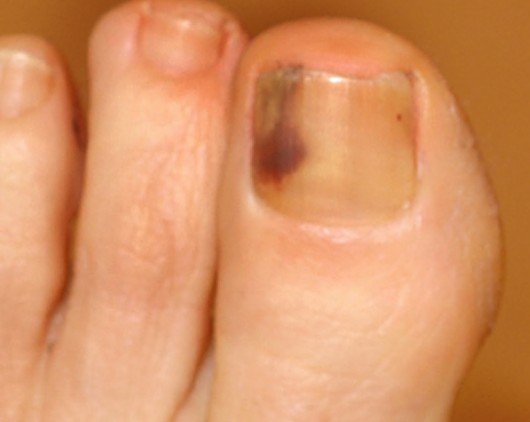
Subungual Melanoma
Subungual melanoma is a type of cancer that involves the nail unit or matrix, hence the name. This type of melanoma is believed to be a variant of other types of cancer, such as: desmoplastic melanoma, nodular melanoma or acral lentiginous melanoma (the latter being the type of cancer that affects the palms of the hands and the soles of the feet). In the majority of the patients, subungual melanoma appears at the level of the big toe nail or at the thumb nail. This has led scientists to believe that trauma might represent a risk factor for the development of subungual melanoma, given the increased incidence of big toe/thumb involvement. However, it is important to remember that any nail can become affected.
This condition is considered to be extremely rare, affecting only 1% of the general white population. The interesting thing is that it affects people of all races, no matter if they are white or dark skinned. In fact, it is one of the most common types of melanomas diagnosed in dark-skinned individuals, even though the incidence is basically the same. In general, subungual melanoma is diagnosed in older individuals and it is believed that not only trauma contributes to its appearance but also prolonged exposure to the sun.
Symptoms of Subungual Melanoma
These are the most common symptoms that are characteristic for the patients with subungual melanoma:
- Wide pigment band appears on the middle of the nail (melanonychia)
- With the progression of the condition, the band will become even wider, especially at the level of the nail cuticle
- The band starts to change its color, becoming more pigmented (dark brown color)
- If the band extends so far as to involve the adjacent nail fold, this is known as the Hutchinson sign
- The nail bed might suffer from changes – nodules or ulcerations may appear, leading to eventual bleeding
- If the nodule is larger in size, it may cause the nail plate to lift (onycholysis)
- The nodule may resemble a wart in appearance (confusion of diagnosis with verrucous lesions)
- The nail plate might start to thin and cracks might appear, distorting the overall appearance of the affected nail (modification known as nail dystrophy)
- No pain is present, with the exception of advanced cases, in which the cancerous growth has reached all the way to the bone (in this case, the patient might suffer from really intense pain)
Keep in mind that, in over half of the patients who suffer from subungual melanoma, there is no pigmented band to draw attention to the problem.
Causes
These are the most common causes that can lead to the appearance of subungual melanoma:
- Trauma to the respective finger/toe (can be acute or chronic)
- Prolonged exposure to the sun
- Inadequate footwear (ill-fitting shoes)
- Foreign body into the finger/toenail
- Radiation therapy for other types of cancer
- Hormonal disorders
- AIDS (Acquired immunodeficiency syndrome)
- Chronic fungal infections of the nail bed
The main two causes incriminated in the appearance of subungual melanoma remain the trauma to the fingers or to the toes (predominantly in the big toe or thumb) and the prolonged exposure to the sun (both factors can be kept under control, thus reducing the risk of subungual melanoma actually appearing).
Diagnosis
These are the most common measures used for the diagnosis of subungual melanoma:
- Medical history of the patient (anamnesis)
- Medication
- Treatments taken in the past
- Illnesses
- Family history of medical problems
- History of trauma to the respective toe/finger
- Prior history of nail biopsies (results as well)
- Number of nails affected
- Bacterial or fungal infections
- Changes of the nails identified over time
- History of longitudinal melanonychia, with recent changes in color, bleeding or ulceration
- Physical examination
- Identification of the pigmented band on the nail (>3mm wide)
- Dermoscopic examination
- Closer look at the pigmented band
- Offers valuable information about the actual color of the band and also determines its width/spacing with precision
- Nail matrix/bed biopsy
- The biopsy is generally used for the confirmation of the diagnosis
- The investigation is performed by a dermatopathologist (difficult diagnosis)
- Useful in determining the type of subungual melanoma (in-situ or invasive)
- The biopsy should provide information about the thickness of the cancerous growth (mm) and also about the other tissues that have been invaded by the melanoma
- Dermoscopy
- Useful to make the differential diagnosis between subungual melanoma and hematoma
The differential diagnosis should be made with the following conditions:
- Subungual hematoma
- Onychomycosis
- Nevus of the nail matrix
- Melanotic macule of the nail unit
The ABCDEF rule is generally used for the diagnosis of the clinical subungual melanoma. This includes: A (age – 40-70), B (brown band, with width over 3mm), C (change in the morphology of the nail bed), D (involvement of the digits), E (extension of the band to the adjacent nail folds) and F (family history of melanoma).
Treatment
These are the most common methods used for the treatment of subungual melanoma:
- Surgical removal
- For the best prognosis, the entire nail apparatus will have to be removed
- May require the amputation of the finger/toe end (distal phalanx amputation)
- Sentinel node biopsy
- Performed in patients who present severe cases of subungual melanoma, so as to determine whether the cancer has spread to the lymph nodes in the area
- Mohs micrographic surgery
- Alternative to the classical surgical removal for subungual melanoma that is in-situ
- The total nail excision, followed by the reconstruction with the full-thickness graft is an option for treatment.
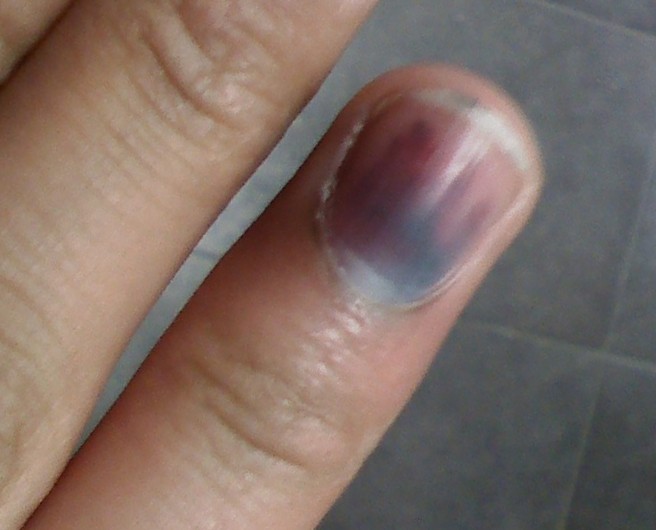
Subungual melanoma vs Hematoma
Subungual hematoma is a medical condition in which a bleeding has occurred under the nail, leading to the appearance of a purple mark on the respective nail. If the doctor cannot confirm for certain whether it is this condition you are suffering from, he/she will monitor the nail for a couple of weeks. With the retraction of the hematoma, the nail will be observed growing healthy, something that does not happen in patients who are suffering from subungual melanoma. The differential diagnosis between subungual melanoma and hematoma can be made with the help of dermoscopy, as the latter does not respect the band-like pattern commonly seen in patients who suffer from subungual melanoma.
Pictures
How does Subungual Melanoma look like?