Leukocytoclastic Vasculitis
What is Leukocytoclastic Vasculitis?
Leukocytoclastic vasculitis is a variant of vasculitis characterized by the inflammation of the tiny blood vessels of the body. The disease often leads to damages in the blood vessels resulting in bleeding and damages of nearby tissues.
Leukocytoclastic vasculitis is also referred as hypersensitivity vasculitis or hypersensitivity angiitis. The disease is presented by small spots of discolorations known as purpura. The spot is caused by the bleeding beneath the skin which in turn causes the reddish or purplish discoloration of the skin.
Vasculitis refers to a group of disease characterized by inflammation of the blood vessels leading to damages in the blood vessels. It is an inflammatory disorder that involves both the veins and the arteries. There are various forms of vasculitis with symptoms that vary significantly and with different duration and severity. The severity of vasculitis ranges from mild to life-threatening and may leave a life-long or permanent damage to the body.
Leukocytoclastic vasculitis is deemed an uncommon disorder. It can affect many people without racial predilection. Men and women are equally affected although some studies revealed a slight prevalence of leukocytoclastic vasculitis among men. The disease can occur at any age with children below the age of 10 years often affected with Henoch-Schonlein purpura.
Leukocytoclastic vasculitis has a good prognosis except when the GI tract, kidney, heart, lungs and the central nervous system are affected. Leukocytoclastic vasculitis not only involves the skin but can also involve the internal organs and the joints. The involvement of the internal organs and the joints are generally a concern which necessitates an immediate medical intervention as this can be life-threatening.
Leukocytoclastic Vasculitis Symptoms
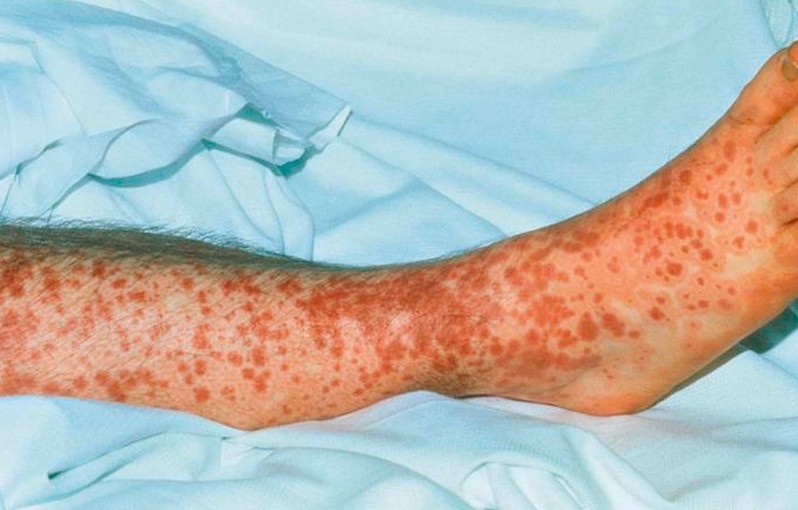
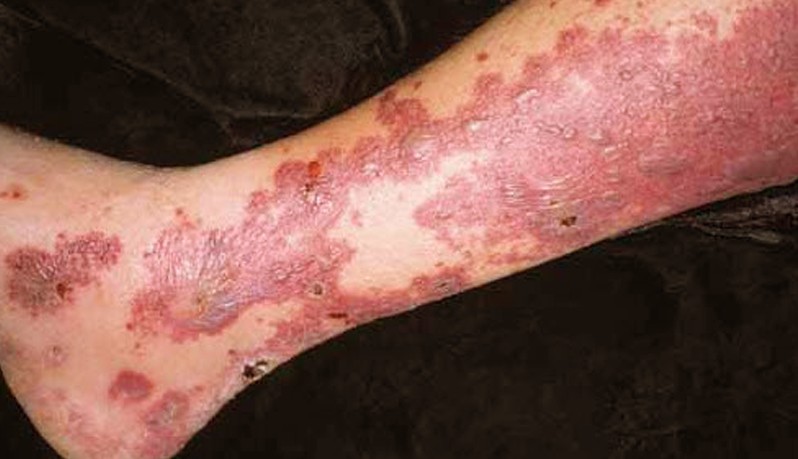
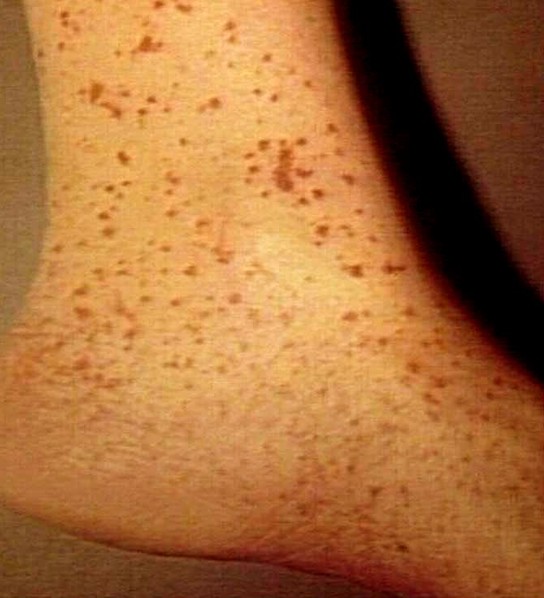
Leukocytoclastic vasculitis is presented by the development of rash in the lower limbs, trunk and buttocks. The inflammation of the tiny blood vessels occurs beneath the skin although there are cases where the internal organs and the joints are also involved in the process of the disease.
A palpable purpura is the most common complaints of patients. The purpura is a reddish or purplish discoloration in the skin that resulted from bleeding under the skin. Purpura is a small spot that is elevated from the skin. The spots may merge together to form a larger spot, although in some cases it may remain small. The purpura may tend to obstruct the flow of blood in the skin leading to necrosis or death of tissue.
The size of the purpura is around 1mm to 3mm in diameter. The lesions can grow bigger when they merge together. In some cases, the purpura may form bullae which can later develop into ulceration. Any areas of the skin can get affected although the common area of development is the lower legs and the areas with trauma and tight fitting clothing. The purpura may not also be palpable although this seldom happens.
In rare cases, urticarial lesions may occur along with leukocytoclastic vasculitis. Urticarial lesion may persist longer than a day and may leave pigmentation. Most patients with the onset of urticarial lesion complain of burning rather than itching.
Leukocytoclastic vasculitis may be presented with pain, itchiness and burning sensation but there are cases where leukocytoclastic vasculitis remains asymptomatic. Some patients with leukocytoclastic vasculitis may experience systemic symptoms such as fever, stomach pains or stomach upset and joint pains. Blisters may develop or there may be the presence of ulceration or open sores. Necrosis is potential especially when the purpura has obstructed the blood flow in the skin leading to deprivation of blood supply in the tissue.
Leukocytoclastic purpura associated with an underlying condition and the signs and symptoms may be reliant or not on the disease process. The signs and symptoms may include the following:
- Onset of fever
- Flu-like symptoms
- Chronic cough
- Abdominal pain or stomach upset
- Presence of blood in the stool
- Diarrhea
- Weakness
- Myalgia or arthralgia
Leukocytoclastic Vasculitis Causes
The majority of cases of leukocytoclastic vasculitis are idiopathic or the cause is unknown. There are identifiable causes however that are being implicated to the onset of leukocytoclastic vasculitis. Leukocytoclastic vasculitis is also being thought to be an error in the immune response where the very blood vessels of the body are mistaken as a foreign object and should therefore be warded off from the body.
Several drugs are considered to be the cause of leukocytoclastic vasculitis and often as an allergic reaction to certain drugs.
Antibiotics
Antibiotics are generally prescribed to inhibit the bacterial growth in the body. There are antibiotics however that can cause leukocytoclastic vasculitis often as an adverse reaction towards the drug.
Other drugs that can cause leukocytoclastic vasculitis include the following:
- Diuretics
- Nonsteroidal anti-inflammatory drugs
- Orlistat
- Letrozole
Several forms of infections can also cause the onset of leukocytoclastic vasculitis.
- Leukocytoclastic vasculitis may occur along with bacterial endocarditis
- Upper respiratory infection is mostly implicated in leukocytoclastic vasculitis especially an infection from beta-hemolytic streptococci
- Viral hepatitis is also among the identifiable cause of leukocytoclastic vasculitis
- Hepatitis C is also commonly implicated to the onset leukocytoclastic vasculitis especially with the presence of cryoglobulinemia
There are some diseases that are being associated with leukocytoclastic vasculitis such as:
Crohn’s disease
Crohn’s disease is an inflammatory bowel disease associated with the onset of leukocytoclastic vasculitis. The inflammation involves the lining of the digestive tract leading to symptoms of abdominal pain and severe diarrhea.
Ulcerative colitis
Ulcerative colitis is also an inflammatory bowel disease that causes abdominal pain and diarrhea. It has also been implicated in the onset of leukocytoclastic vasculitis.
Food additives and other substances can also cause the incidence of leukocytoclastic vasculitis.
Leukocytoclastic Vasculitis Treatment
It is important to establish the diagnosis first prior to the treatment of leukocytoclastic vasculitis. The patient has to be carefully evaluated and the cause of the disease should be identified first to determine the proper treatment necessary.
The treatment of leukocytoclastic vasculitis depends on the overall health status of the patient and the underlying cause.
The general measures for treating leukocytoclastic vasculitis include the following:
- Elevation of the affected leg or legs or wearing of compression stockings are beneficial
- Immediate discontinuation of the drug that causes leukocytoclastic vasculitis is required although a visit to the doctor is necessary to discuss the condition prior to discontinuation of the medicine
The pharmacological treatment of leukocytoclastic vasculitis includes the following:
- Colchicines or dapsone
- Antihistamine
- Non-steroidal anti-inflammatory drugs
- Prednisolone
- Broad spectrum steroid
- Immunosuppressive drugs
Leukocytoclastic Vasculitis Pictures
Collection of photos, images and pictures of Leukocytoclastic Vasculitis…