Enthesopathy
What is Enthesopathy?
Whenever a health problem occurs at the level of a tendon or a ligament’s insertion on the bone, this condition is known as enthesopathy. The name derives from the fact that the insertion site is presented in medical terms as entheses. When inflammation appears as part of the process, the condition will be known as enthesitis.
As you will have the opportunity to see below, enthesopathy can appear at different levels of the body, including in the spine, upper and inferior extremities. When it comes to occurs at the level of the vertebral column, it is generically presented as spondyloarthropathies (ankylosing spondylitis is one of the most common types of spondyloarthropathy, affecting primarily men).

At the level of the upper extremities, enthesopathy can appear under the following forms: adhesive shoulder capsulitis (frozen shoulder), rotator cuff syndrome, periarthritis (shoulder involvement), fibrositis with involvement of the shoulder and scapula, hand/wrist synovitis, wrist periartritis. As for the inferior extremities, the most common forms include: tendinitis (gluteal, psoas or trochanteric) and spurs at the level of the iliac crest.
Enthesopathy Symptoms
These are the general symptoms of enthesopathy:
- Inflammation (acute or chronic) → can modify the aspect of certain anatomical structures (if severe) → sausage-like aspect of the fingers or toes (for example)
- Pain → nerve endings of entheses → enthesalgia → chronic musculoskeletal pain
- Abnormal calcification/ossification → entheses level
- Irritation at the level of the affected tendon or ligament attachment
- Soreness can also be present among the symptoms
- The symptoms can be intermittent (come and go)
- Recurring stress → more inflammation → calcification and fibrosis
- Because of the pain, inflammation and soreness, the patient might not be able to perform regular activities (for example, if the Achilles tendon is affected, he/she will have difficulties walking or running).
Causes of Enthesopathy
These are the most common causes that lead to the appearance of enthesopathy:
- Inflammatory conditions
- Psoriatic arthritis
- Reactive arthritis
- Rheumatoid arthritis
- Osteoarthritis
- Crohn’s disease
- Reiter’s syndrome
- Tennis elbow/golfer elbow
- Postman’s heel
- Iliotibial band syndrome
- Physical injury or trauma
- Excess load
- Plantar fasciitis
- Other causes
- Diffuse idiopathic skeletal hyperostosis
- Medication (side-effect)
- Drug abuse
- Infection
- Metabolic change.
Enthesopathy Treatment
These are the general measures of treatment recommended for enthesopathy:
- Anti-inflammatory medication
- Topical or oral administration (depending on the severity of the pain and inflammation)
- Reduce the inflammation and bring the necessary pain relief
- Recommended choices – acetaminophen, ibuprofen, naproxen
- Corticosteroid injections
- Recommended in the situation that the above-mentioned anti-inflammatory medication has failed to provide the desired results
- Anti-TNF agents
- Recommended for patients who suffer for more serious cases, with severe inflammation
- Indicated choices – Humira, Remicade and Enbrel
- Radiotherapy
- Beneficial effects for patients who suffered from affectation at the level of the heel
- Other treatment solutions
- Combination of sulfasalazine and methotrexate
- Heel inserts (for patient who suffer from plantar fasciitis)
- Physical therapy
- Occupational therapy
- Ultrasound
- Electrical stimulation
- Ice application (wrapped in a towel, not directly on the skin).
Enthesopathy of hip
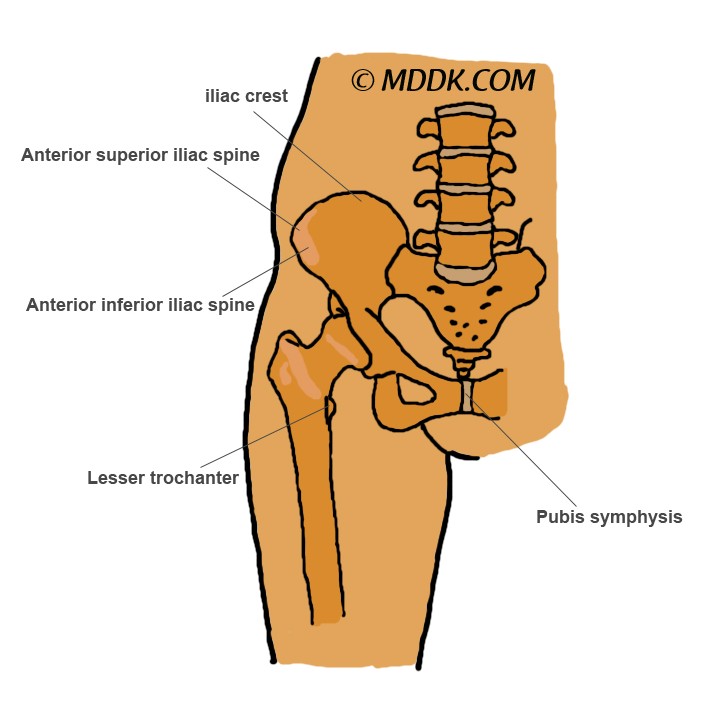
Picture of Enthesopathy of the hip
When a person suffers from the enthesopathy of the hip, this means that insertion of the tendons or ligaments at the level of the hip bone sockets have been affected. This is an arthritic disorder and it may impair the proper functioning of the hip, leading to reduced range of motion and pain. The patient might experience difficulties when trying to walk or move in general.
At the insertion of the hip muscles tendons or ligaments, one can either see calcification or ossification. The articular capsule is the least affected by the enthesopathy. X-ray investigations demonstrate characteristic changes at the level of the femoral head and also at the joint acetabulum. Severe cases of hip enthesopathy, such as the greater trochanteric bursal pain, can be successfully treated with platelet-rich plasma (provided other treatments have failed to provide the desired results).
Spinal enthesopathy
When talking about spinal enthesopathy, one talks about medical conditions, such as ankylosing spondylitis. Because of the chronic inflammation, in time, the ligamentous insertions to the spine are damaged. The more the ligaments are eroded, the more the bone will try to compensate through calcification or ossification. The treatment for spinal enthesopathy includes the administration of non-steroidal anti-rheumatic medication.
It is possible that a non-inflammatory form of enthesopathy appears at the level of the spine, this being known as ankylosing vertebral hyperostosis. This hyperostotic disease can cause the insertions of the spinal ligaments to become ossified, leading to the appearance of intervertebral bridges. Once these bridges have been formed, the patient will start to experience the first symptoms: pain and rigidity at the level of the neck and back, with reduced range of motion. In more severe cases, it is possible that the patient suffers from the compression of the spinal cord at cervical level or from the stenosis of the lumbar canal. The overall mobility of the spine can be reduced, with the combination of changes leading to the appearance of secondary osteoarthritis.
Spinal enthesopathy can also be present in patients who suffer from psoriatic arthritis, leading to back pain and a wide range of other symptoms. The back pain is chronic, having a gradual onset and improving with physical movement. Characteristic for this kind of problem is the fact that the pain does not improve with physical rest. The pain can keep the patient awake at night, the level of stiffness being at maximum in the morning. In general, this form of spinal enthesopathy is diagnosed in men who are over 40 years of age.
The treatment options include physical therapy, the administration of non-steroidal anti-inflammatory medication and intramuscular corticosteroid injections. Sulphasalazine might be used to provide relief from the pain but it is not effective in all of the patients. Anti-TNF therapy remains the standard treatment for those who suffer from more severe forms.
Achilles tendon enthesopathy
When the insertion of the Achilles tendon is affected, the condition is known as Achilles tendon enthesopathy. This condition occurs because of constant traction of the respective muscle tendon on the calcaneus bone. Being sedentary or obese are considered as risk factors for such health problems, as they lead to the shortening of the calf muscles (or to their chronic contracture). The patient presents pain at the level of the posterior heel, especially during walking. The pain is exacerbated by the palpation of the tendon at its insertion point. The same goes for the manual dorsiflexion of the ankle.
There are three treatment recommended for Achilles tendon enthesopathy, meaning physical therapy (stretching), splinting and heel lifts. Physical therapy is essential, as it can help one stretch the shortened calf muscles and eliminate the contractures that are present at this level. Night splints can also be used, having the purpose of passively stretching the shortened calf muscles during sleep. These are considered as one of the best ways to prevent additional contractures. The usage of heel lifts is recommended to be only temporary, as they can relieve the stress experienced by the heel during weight bearing. Heel lifts can alleviate the pain experienced by the patient, improving the gait and avoiding the compensatory movements of the hip (these can have a harmful effect, leading to low back pain).